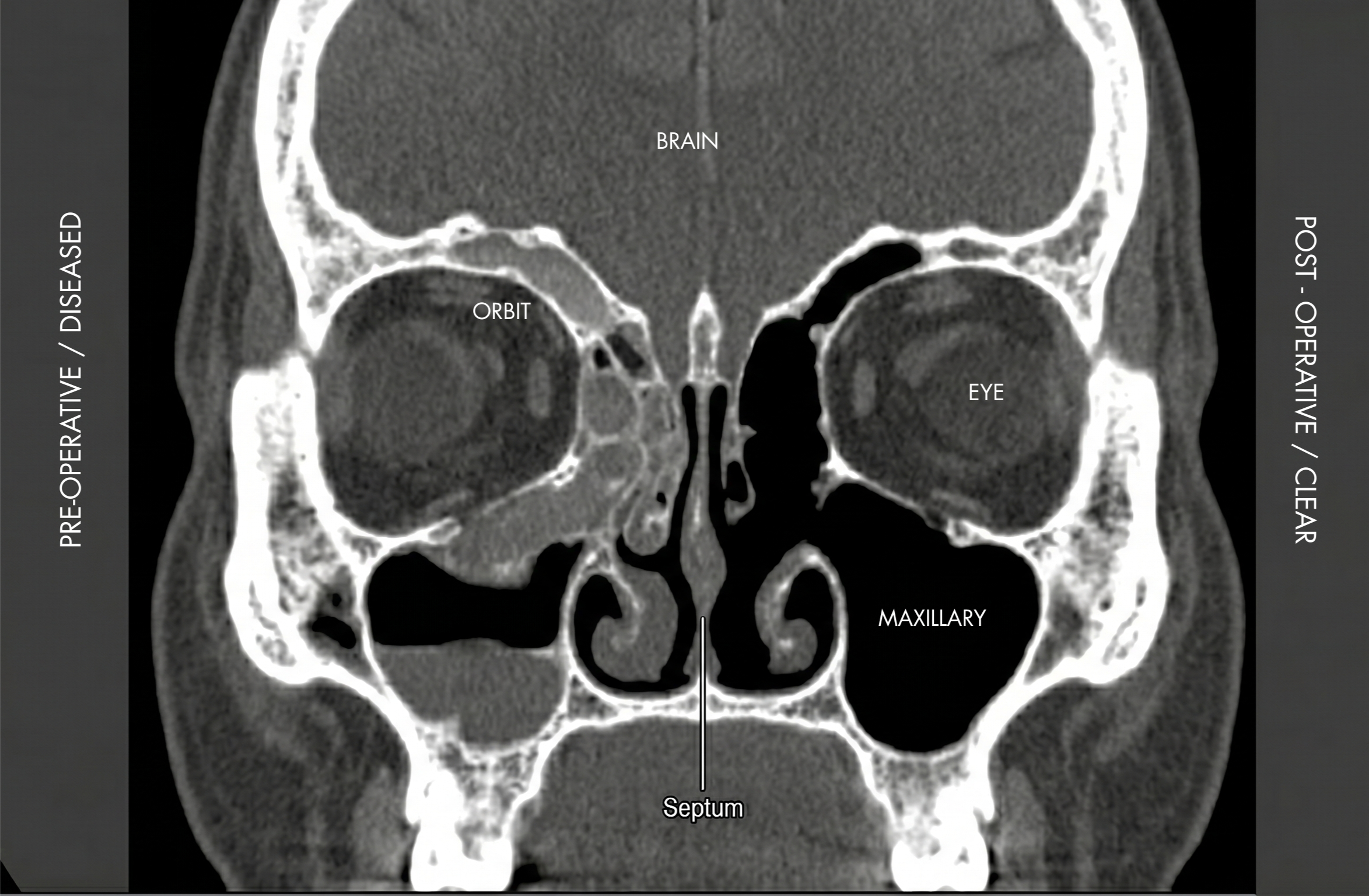
| FESS (Functional Endoscopic Sinus Surgery) |
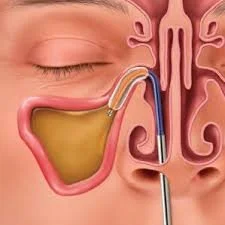
Balloon Sinuplasty |
| A surgery that uses small instruments and a camera to remove bone, tissue, and polyps to permanently open blocked sinus passages. |
A less invasive procedure that uses a small balloon catheter to stretch open blocked sinus passages — no tissue or bone is removed. |
| Operating room (hospital or surgery center) |
Can be done in the doctor's office OR in an operating room |
| Usually general anesthesia (you are fully asleep) |
Often local anesthesia only (you are awake but numb); sometimes general anesthesia |
| Approximately 1–2 hours |
Approximately 30 minutes |
| About 1–2 weeks off work (average ~8 sick days) |
About 2–4 days off work (average ~3-4 sick days) |
| Moderate — nasal packing may be used; expect congestion, pressure, and discomfort for 1–2 weeks |
Mild — usually less pain and congestion; most patients return to normal activities within 1–2 days |
| Bleeding, infection, scarring/adhesions inside the nose, eye injury (rare), spinal fluid leak (rare) |
Bleeding, infection, eye injury (rare), spinal fluid leak (rare); overall complication rate is lower |
| Very effective — considered the gold standard for chronic sinusitis; proven long-term results |
Effective — studies show similar improvement compared to FESS for patients without nasal polyps |
| About 6% may need revision surgery within 10 years |
About 6% may need revision surgery within 10 years |
| More complex sinus disease, nasal polyps, deviated septum, or when tissue/bone needs to be removed |
Milder or limited sinus disease without nasal polyps |
| Lower device cost, but higher facility/anesthesia fees (operating room); total ~$4,000–$7,000+ |
Higher device cost, but lower facility fees if done in-office; total ~$3,000–$6,000+ |
| Usually covered by insurance for chronic sinusitis |
Usually covered by insurance, but coverage may vary |
| ✔ Can treat all types of sinus disease, including polyps ✔ Proven long-term track record ✔ Can address structural problems (deviated septum, etc.) |
✔ Less invasive — no tissue removal ✔ Can be done awake in the office ✔ Faster recovery and less time off work ✔ Lower complication rate ✔ Less scarring inside the nose |
| ✘ Requires general anesthesia in most cases ✘ Longer recovery ✘ Higher risk of scarring/adhesions ✘ More post-op visits and medications needed |
✘ Cannot remove polyps or correct structural problems ✘ Not suitable for severe or complex disease ✘ Device costs may be higher ✘ Long-term data still evolving |